TNF Inhibitor Cancer Risk Assessment Tool
Your TNF Inhibitor Risk Profile
This tool provides personalized assessment of cancer risk based on your specific TNF inhibitor and medical history. Results are based on current clinical research.
0.98 hazard ratio compared to non-biologic drugs
Consistently shows lowest cancer risk across studies
1.3x higher non-melanoma skin cancer risk
May be higher for patients with sun damage or prior skin cancer
No Fc portion may reduce immune suppression
Promising for cancer history patients
Skin Cancer Risk
Your Assessment
Based on your inputs, your risk profile is Low. This means:
- Overall cancer risk remains similar to patients not using biologics
- Regular skin checks every 6-12 months are recommended
- No contraindications to continue your current TNF inhibitor
Consideration: If you have a history of skin cancer, discuss switching to etanercept or certolizumab with your rheumatologist.
Important Note
These results are based on current clinical data and should be discussed with your rheumatologist or oncologist. Individual risk factors may vary based on your complete medical history.
Always follow your healthcare provider's recommendations for monitoring and treatment.
When you're living with rheumatoid arthritis, psoriatic arthritis, or inflammatory bowel disease, the goal isn't just to manage pain-it's to stop your body from destroying itself. That's where TNF inhibitors come in. These drugs, part of a class called biologics, have changed the game for millions. But with great power comes great concern: does using them raise your risk of cancer?
The short answer? It's complicated. For most people, the benefits far outweigh the risks. But not all TNF inhibitors are the same, and not all patients face the same level of risk. Let’s break it down-no jargon, no fluff, just what you need to know.
What Are TNF Inhibitors, Really?
TNF stands for tumor necrosis factor. It’s a protein your immune system makes to fight infection. But in autoimmune diseases, it goes haywire and starts attacking your joints, skin, or gut. TNF inhibitors block this protein, calming down the chaos.
Five of these drugs are FDA-approved and widely used today:
- Infliximab (Remicade)
- Etanercept (Enbrel)
- Adalimumab (Humira)
- Certolizumab pegol (Cimzia)
- Golimumab (Simponi)
They’re not pills. You get them as injections or IV infusions. Some are given weekly, others every few weeks. They cost between $4,500 and $6,500 a month-yes, that’s real. But for many, the trade-off is worth it: fewer flares, less joint damage, and the ability to work, play, and live normally again.
Do TNF Inhibitors Cause Cancer?
This is the question everyone asks. The fear isn’t unfounded. In 2008, the FDA added a black box warning to all TNF inhibitors for lymphoma and other cancers. That warning still exists. But here’s what the long-term data actually shows.
A 2022 study tracking over 15,700 rheumatoid arthritis patients in Sweden found no overall increase in cancer risk from TNF inhibitors compared to older, non-biologic drugs. The hazard ratio? 0.98-meaning no increased risk. That’s a big deal. But digging deeper, the story gets more nuanced.
Adalimumab showed a slight spike in cancer risk during the first year of treatment. That sounds scary, but experts think it’s not because the drug causes cancer. It’s more likely that people who were already developing cancer-undetected-were starting treatment. This is called protopathic bias. The cancer was already there. The drug didn’t cause it.
Etanercept, on the other hand, showed a lower cancer risk than patients who never used biologics. Why? We don’t fully know. But it’s consistent across multiple studies.
For skin cancer, the risk is real-but small. A 2021 analysis of over 32,000 psoriasis patients found a 32% higher rate of non-melanoma skin cancer (like basal cell and squamous cell carcinomas). That’s not trivial. But there was no increase in lung, breast, or colon cancer. And here’s the kicker: patients who used TNF inhibitors and later developed lung cancer had better survival rates than those who didn’t. Why? Possibly because their inflammation was better controlled, or because they were monitored more closely.
Not All TNF Inhibitors Are Created Equal
Here’s where it gets practical. If you’re choosing between adalimumab and etanercept, the data points to a clear difference.
A 2021 meta-analysis in the British Journal of Dermatology found that adalimumab carries a 1.3 times higher risk of non-melanoma skin cancer than etanercept. That’s not a huge jump, but for someone with a history of sun damage or previous skin cancers, it matters.
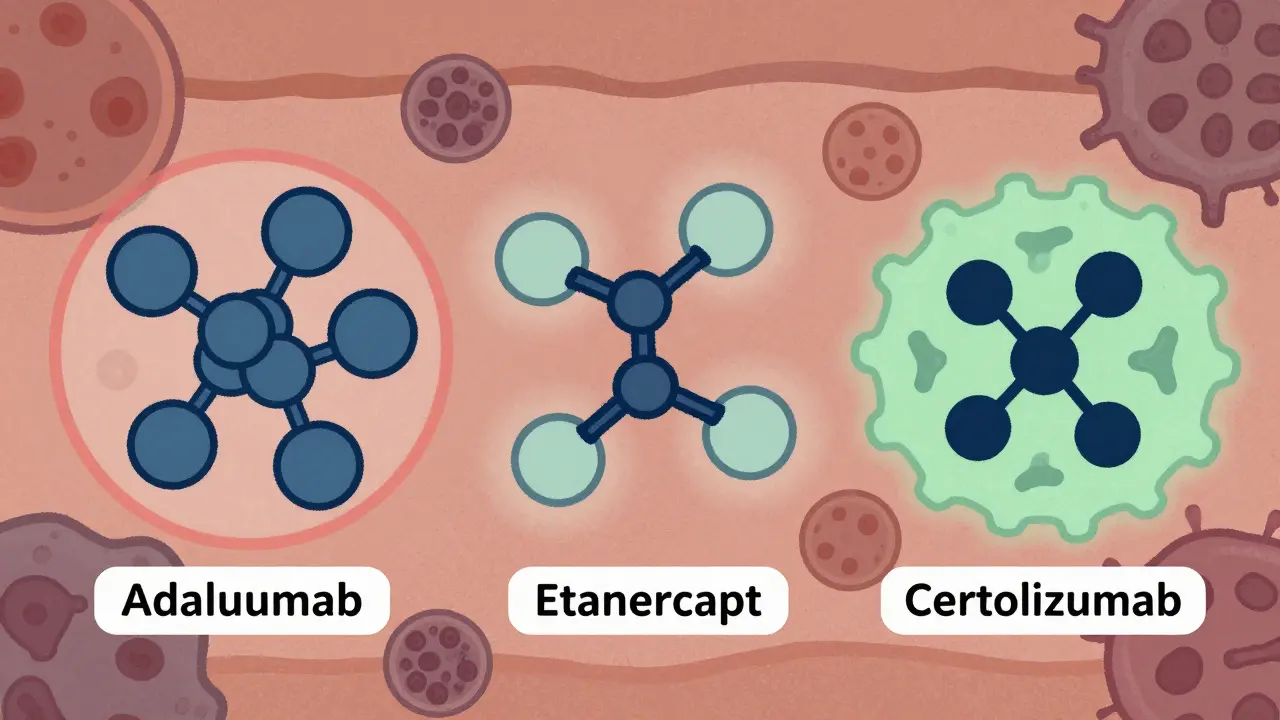
Why the difference? It comes down to how the drugs work. Adalimumab and infliximab are monoclonal antibodies that bind tightly to TNF. Etanercept is a fusion protein that’s more flexible. Some researchers think etanercept may allow some TNF activity to remain-enough to help the immune system spot early tumors.
And then there’s certolizumab. It’s the only one without a Fc portion (a part of the antibody that interacts with immune cells). Early data suggests it might be the safest option for patients with a history of cancer, but we need more long-term studies.
Who Should Be Extra Cautious?
Not everyone is a good candidate. The American College of Rheumatology (ACR) guidelines are clear:
- Don’t start TNF inhibitors if you have active infections (like tuberculosis or hepatitis B).
- Avoid them if you have advanced heart failure or multiple sclerosis.
- If you’ve had cancer in the past, wait at least 5 years after treatment for high-risk cancers like melanoma or lymphoma. For low-risk cancers like early-stage breast or prostate cancer, 2 years is enough.
And don’t forget about steroids. If you’re still on prednisone at 7.5 mg or more per day, your cancer risk goes up. A 2023 study found patients on high-dose steroids had nearly triple the risk of dying from cancer after diagnosis. The solution? Use TNF inhibitors to get off steroids-not just add them on.
What Do Real Patients Say?
Online forums and patient surveys tell a story that numbers alone can’t capture.
A 2022 analysis of 478 posts on the Rheumatology subreddit showed:
- 63% of patients worried most about skin cancer.
- 28% had basal cell carcinomas detected during treatment-caught early by routine dermatology checks.
- 41% said TNF inhibitors gave them their life back.
- 19% stopped treatment because their doctor advised it due to past cancer history.
The National Psoriasis Foundation surveyed 1,200 patients in 2023. The results? 78% would restart a TNF inhibitor after early-stage cancer treatment. Why? Because they trusted their doctors, had regular skin checks, and saw how much better they felt.

What Should You Do?
If you’re considering a TNF inhibitor-or already on one-here’s your action plan:
- Get screened before starting. Ask for a full skin exam, mammogram (if applicable), colonoscopy, and TB test. Don’t skip it.
- Know your drug. If you’re on adalimumab and have a history of sun damage or skin cancer, talk to your rheumatologist about switching to etanercept or certolizumab.
- Get skin checks every 6 to 12 months. Even if you’ve never had skin cancer. Dermatologists can catch early lesions before they spread.
- Stop or reduce steroids. If you’re still on prednisone, work with your doctor to taper it off. It’s one of the biggest modifiable risks.
- Don’t panic about the black box warning. It’s there because regulators have to warn about everything. The real risk for most people is low.
And if you’ve had cancer? You’re not out of luck. A 2023 Corrona registry study found that 87% of rheumatologists continue TNF inhibitors in patients with early-stage solid tumors-after consulting with an oncologist. And 92% of those patients had no cancer recurrence linked to the drug.
The Bottom Line
TNF inhibitors don’t cause cancer. They don’t magically turn your immune system into a cancer-promoting machine. But they do change how your body watches for trouble. That’s why monitoring matters more than ever.
The data is clear: for most people, the risk of uncontrolled inflammation-joint destruction, organ damage, disability-is far greater than the risk of cancer from the drug.
And if you’re worried? Talk to your rheumatologist. Bring this article. Ask about your specific drug. Ask about skin checks. Ask about steroid use. You have the right to understand your treatment. And with the right information, you can make a choice that gives you not just relief-but peace of mind.
Do TNF inhibitors cause cancer?
No, TNF inhibitors do not directly cause cancer in most people. Long-term studies tracking over 15,000 patients show no overall increase in cancer risk compared to older arthritis drugs. However, there is a small, temporary increase in non-melanoma skin cancer risk, especially with adalimumab. The black box warning from the FDA is based on theoretical risk and rare cases, not widespread evidence. For most patients, the benefits far outweigh the risks when monitored properly.
Which TNF inhibitor has the lowest cancer risk?
Etanercept (Enbrel) has the lowest cancer risk among TNF inhibitors. Multiple studies show it doesn’t increase overall cancer risk and may even lower it compared to patients not on biologics. It also carries a lower risk of non-melanoma skin cancer than adalimumab or infliximab. This may be due to its different molecular structure, which allows some natural TNF activity to remain, helping immune surveillance.
Can I take a TNF inhibitor if I’ve had cancer before?
Yes, in many cases. The American College of Rheumatology recommends waiting at least 2 years after successful treatment for low-risk cancers like early breast or prostate cancer, and 5 years for high-risk cancers like melanoma or lymphoma. After that, many rheumatologists safely restart TNF inhibitors-especially if you’re cancer-free and under regular monitoring. A 2023 study found 87% of doctors continued TNF therapy in patients with early-stage cancer, with no increased recurrence.
How often should I get skin checks while on a TNF inhibitor?
Every 6 to 12 months. Even if you’ve never had skin cancer, regular dermatology exams are critical. Non-melanoma skin cancers (like basal cell carcinoma) are common and treatable if caught early. The National Psoriasis Foundation recommends biannual skin checks for all patients on TNF inhibitors. Some doctors suggest monthly self-checks for new or changing moles, especially if you’re on adalimumab or have fair skin.
Are biosimilars safer than brand-name TNF inhibitors?
Yes, biosimilars are just as safe. Biosimilars like adalimumab-bwwd (Abrilada) are highly similar to the original drug in structure, function, and safety profile. The FDA requires them to meet strict standards before approval. There is no evidence that biosimilars carry a higher cancer risk than brand-name versions. In fact, their lower cost may improve access to regular monitoring, which can reduce overall cancer risk.
What’s Next?
The future of TNF inhibitors isn’t about stopping them-it’s about personalizing them. By 2027, doctors may use genetic tests to identify patients at 3.2 times higher risk for lymphoma based on their DNA. That’s not science fiction-it’s already in clinical trials.
For now, the message is simple: don’t let fear stop you from living. With smart screening, careful drug choice, and regular checkups, TNF inhibitors remain one of the safest and most effective tools we have for autoimmune disease.
jared baker
March 18, 2026 AT 17:02
For anyone scared of cancer risk from TNF inhibitors, let me say this: the real danger is leaving your RA or psoriasis untreated. I’ve seen friends go from walking with canes to hiking mountains after starting Humira. The skin cancer risk? Manageable. Get yearly checks, wear sunscreen, and don’t panic. The data doesn’t support fear-it supports action.
Paul Ratliff
March 18, 2026 AT 19:35
adalimumab is a nightmare for skin cancer. i got 3 bccs in 18 months. switched to enbrel and zero new ones. doc said it’s the fce part. no idea what that means but my skin loves it now.
SNEHA GUPTA
March 19, 2026 AT 08:19
It’s fascinating how we fear what we don’t fully understand. TNF inhibitors don’t cause cancer-they reveal the fragility of our immune surveillance. The body was already on the edge. The drug didn’t push us over. It just made us look closer. And that’s not a flaw. It’s a feature.
Gaurav Kumar
March 20, 2026 AT 17:24
Why are Americans so scared of everything? In India, we use these drugs without panic. You think cancer? We think relief. Your healthcare system turns medicine into a horror story. Etanercept is safe. Get over it. 🤦♂️
David Robinson
March 21, 2026 AT 18:08
Wait, so you’re telling me a drug that suppresses your immune system doesn’t increase cancer risk? That’s not science, that’s wishful thinking. I’ve read studies where immunosuppressants increased lymphoma rates by 400%. You’re ignoring the outliers. The FDA didn’t put a black box warning for fun. You’re lucky if you’re one of the 98%.
Jeremy Van Veelen
March 23, 2026 AT 16:40
Let me be blunt: if you’re on a TNF inhibitor and you’re not getting skin checks every six months, you’re playing Russian roulette with your life. This isn’t a medical decision-it’s a moral one. Your skin is your first line of defense. Neglect it, and you’re not just risking cancer-you’re disrespecting the science that gave you your life back.
Laura Gabel
March 24, 2026 AT 20:15
my dermatologist said i need checks every 6 months. i did it for a year then stopped. no new moles. prob fine. dont need to be paranoid
jerome Reverdy
March 26, 2026 AT 06:08
Look, the data’s clear: etanercept is the safest bet for long-term use, especially if you’ve got a history of sun exposure. Adalimumab? Higher skin cancer risk, no question. But here’s the kicker-it’s not about the drug. It’s about the person. Your age, your skin type, your family history, your sun habits. That’s the real variable. The drug’s just the tool. Use it wisely.
Andrew Mamone
March 27, 2026 AT 01:16
Just switched from Humira to Enbrel last month. 🌞☀️☀️☀️ Went from monthly skin checks to every 6 months. My derm said my lesions are healing better too. The science is real. Trust the data, not the fear. 💪
MALYN RICABLANCA
March 28, 2026 AT 12:09
Oh my GOD, I can’t believe this article is downplaying the risk?! I had a melanoma removed while on Cimzia-my oncologist said it was likely triggered by the drug! I lost my hair, my confidence, my job! And now you’re telling me to just ‘get a skin check’?! This isn’t a lifestyle choice-it’s a life-or-death gamble! And don’t even get me started on steroids! I was on 15mg of prednisone for 3 years! I’m lucky I’m alive!
gemeika hernandez
March 30, 2026 AT 05:21
My cousin went on Humira and got skin cancer. She died. Don’t listen to these ‘studies.’ Real people die. You think numbers matter? They don’t. Not when it’s your mom, your sister, your best friend. Stop being so clinical. This isn’t a spreadsheet.
Prathamesh Ghodke
March 31, 2026 AT 13:01
Actually, the fact that etanercept might allow some TNF activity to remain is a brilliant evolutionary hack. It’s not about fully blocking inflammation-it’s about fine-tuning it. Like a dimmer switch instead of an on/off button. That’s why it’s safer. The body still has a little watchtower up. Smart design.
Stephen Habegger
April 1, 2026 AT 22:40
Been on Enbrel for 7 years. No cancer. No flares. Just a normal life. If you’re scared, talk to your doc. But don’t let fear steal your joy. You’ve already fought enough.
jared baker
April 2, 2026 AT 17:00
@8082 Totally agree. The idea that some TNF activity helps with immune surveillance is why I switched from adalimumab. My rheumatologist called it ‘leaky inhibition’-sounds weird, but it makes sense. Your immune system needs a little wake-up call, not a full lockdown.
Kyle Young
April 4, 2026 AT 04:53
What’s fascinating is how the biological mechanism of etanercept-being a fusion protein rather than a monoclonal antibody-creates a more dynamic interaction with TNF. It doesn’t fully neutralize it, which may preserve immune surveillance pathways critical for tumor detection. This isn’t just pharmacology-it’s immunological elegance.